Deadly New Ebola Strain Emerges in Congo: Concerns Mount Over Undetected Spread in Conflict Zone
By [Your Name], International Health Correspondent
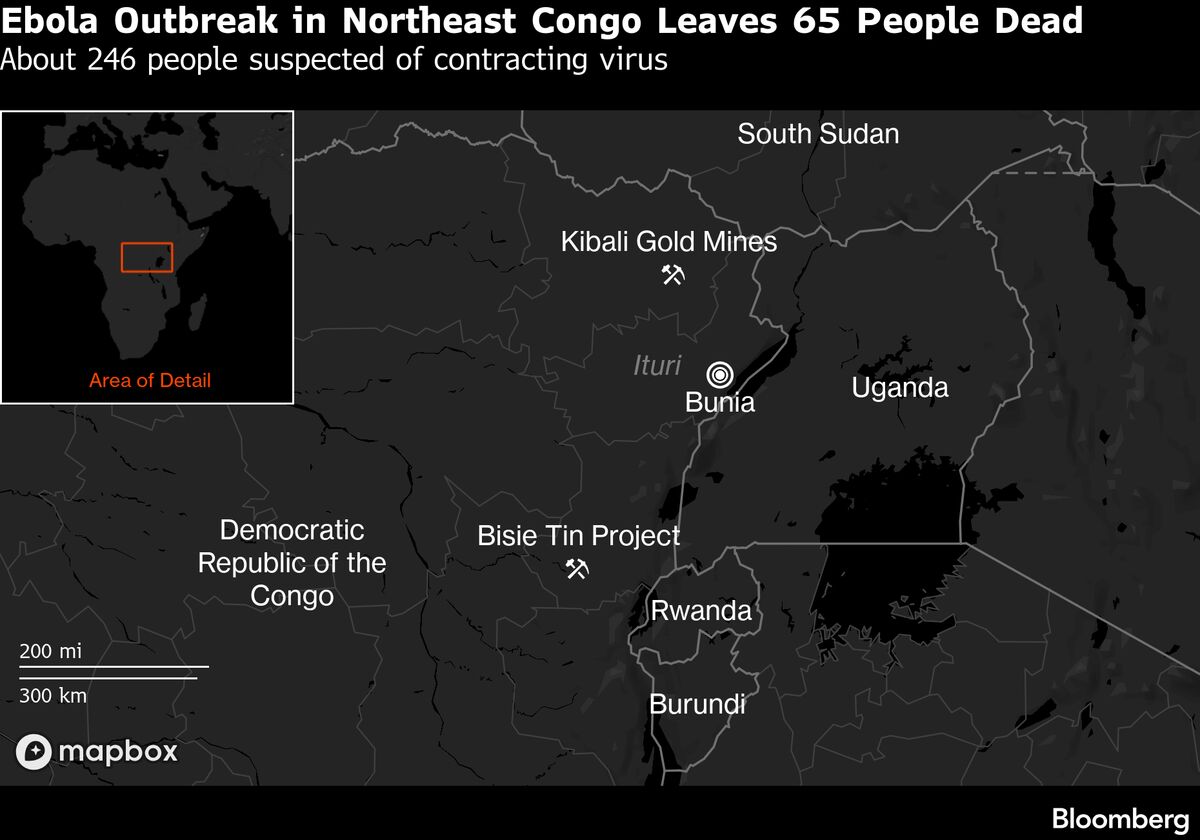
GOMA, Democratic Republic of Congo — A previously undocumented and highly lethal strain of Ebola, for which no vaccines or treatments exist, is suspected to have spread undetected for weeks in the war-torn northeastern regions of the Democratic Republic of Congo (DRC), raising fears of a potential public health crisis. At least two dozen deaths have already been linked to the outbreak, with health officials scrambling to contain its spread in an area plagued by armed conflict, poor infrastructure, and deep community mistrust of authorities.
The outbreak, first identified in late April but believed to have begun circulating earlier, involves a rare genetic variant of the Zaire ebolavirus—one of the deadliest pathogens known to humanity. Unlike previous Ebola epidemics, this strain lacks any approved countermeasures, leaving medical teams reliant on basic containment protocols in a region where access is severely restricted due to ongoing violence. The World Health Organization (WHO) has classified the situation as “high risk,” warning that delayed detection and the region’s instability could complicate efforts to stem the outbreak before it escalates further.
A Perfect Storm: Conflict and a Stealthy Pathogen
The northeastern DRC, particularly the provinces of North Kivu and Ituri, has been a hotspot for Ebola outbreaks in recent years, including the 2018-2020 epidemic that claimed over 2,200 lives. However, this new strain presents unprecedented challenges. Genetic sequencing suggests it diverges significantly from known variants, meaning existing vaccines—such as Merck’s Ervebo, which proved effective in prior outbreaks—may offer little to no protection.
Compounding the danger is the region’s protracted humanitarian crisis. Decades of militia violence, including attacks by groups such as the Allied Democratic Forces (ADF), have displaced millions and crippled healthcare systems. Many villages remain cut off from aid, allowing diseases to fester unnoticed. “This is a worst-case scenario,” said Dr. Jean-Jacques Muyembe, a renowned Congolese virologist who helped discover Ebola in 1976. “When cases go unreported due to insecurity, the virus gains a head start.”
Silent Spread: How the Outbreak Evaded Detection
Preliminary epidemiological investigations suggest the virus may have been circulating since at least March, with early cases misdiagnosed as malaria or typhoid—common ailments in the region with overlapping symptoms. By the time blood samples confirmed Ebola in late April, at least 35 suspected cases had been reported across several remote villages, with a fatality rate exceeding 60%.
Local health workers describe harrowing conditions. “Patients were dying before we even knew what we were dealing with,” said a nurse in Beni, one of the affected towns, who requested anonymity for safety reasons. “Without proper diagnostics, it was like fighting shadows.”
The lack of roads, coupled with frequent militia roadblocks, delayed sample transport to laboratories in Goma and Kinshasa. By then, the virus had likely spread through traditional burial practices, where mourners touch the deceased—a known transmission route for Ebola.
Global Alarm and the Race for Solutions
The WHO has deployed emergency response teams, but their movements are constrained by security protocols. “We’re operating in a war zone,” said Dr. Mike Ryan, head of the WHO’s Health Emergencies Programme. “Every delay costs lives.”
Scientists are urgently studying the strain to determine whether experimental therapies, such as monoclonal antibodies used in past outbreaks, could be adapted. Meanwhile, pharmaceutical companies are exploring accelerated vaccine development, though regulatory approvals could take months.
The DRC’s government, with support from the Africa Centres for Disease Control (Africa CDC), has launched a contact-tracing campaign and public awareness drives. Yet distrust of outsiders remains high—fueled by rumors and past mismanagement of aid. “Communities hide sick relatives because they fear hospitals are death traps,” said Dr. Guyguy Manangama of Médecins Sans Frontières (MSF).
A Test for Global Health Preparedness
This outbreak underscores the vulnerabilities of pandemic preparedness in conflict zones. Despite advances since the 2014-2016 West Africa Ebola crisis, which killed 11,000, gaps persist in surveillance and equity. “We cannot keep waiting for outbreaks to spiral before acting,” said Dr. Matshidiso Moeti, WHO Regional Director for Africa.
The international community faces a dilemma: intervene aggressively despite risks to personnel, or risk regional spillover. Neighboring Uganda, still recovering from a 2022 Ebola outbreak, has heightened border screenings.
A Fragile Hope
For now, health workers brace for a prolonged battle. “We’re rebuilding trust, case by case,” said North Kivu’s health minister, Dr. Michel Tosalisana. But with each day of violence and logistical hurdles, the virus gains ground.
As the world watches, the question remains: Can science and solidarity outpace a pathogen in one of the planet’s most volatile corners? The answer may define the next chapter of global health security.